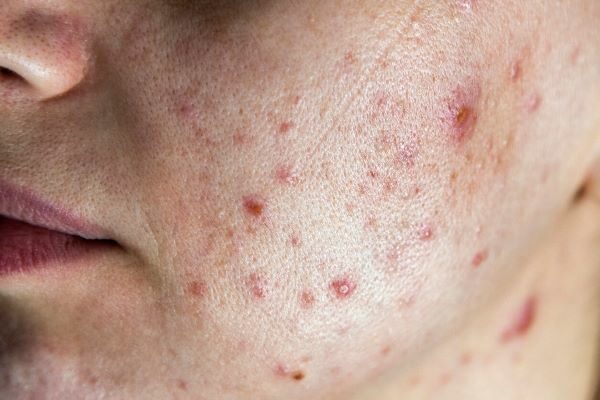
If you have come across mixed opinions about hormonal acne or acne in general, then best believe it – you are not alone! The good news is that there are effective treatment options for how to manage hormonal acne.
Some misperceptions or skepticism surrounding acne include the role of diet in acne, the causes of acne, and the effectiveness of available treatment or management of acne which may be cosmeceutical, medical, hormonal, etc.
Disclaimer: This is not intended to be medical advice but informational only. This article is a product of the author’s research, knowledge, and private consultations with some health professionals.
WHO IS AFFECTED BY ACNE
Acne affects approximately 80% of adolescents and young adults from age 11 up to age 30, says Elsaie. While many will no longer suffer acne before they turn 30 years of age, the rest will continue to suffer acne of different forms.
Since acne differs in presentations including the likely factors that contribute to its formation, there have been attempts to categorize the different types of acne.
While this article will focus on hormonal acne, clarify what hormonal acne is about as well as available treatments you can explore, you may find it helpful to have some understanding of the different types of acne and contributing factors.
WHAT ARE THE BASIC TYPES OF ACNE?
Several attempts have been made to categorize acne but they all fall into the following;
1) Adolescent acne: Also referred to as teen acne depending on your source of information.
2) Persistent, Recurring or Late Acne Onset: These are used as references to whether adolescent acne is persistent into adulthood or whether acne remits in adolescence and then re-occurs in adulthood or whether acne occurs for the first time (late onset) in adulthood.
3) Adult Acne – Affects both males and females in adulthood but mostly females (termed adult female acne or “hormonal acne”).
WHAT COMMONLY OCCURS DURING ACNE FORMATION
Whether you have adolescent or adult acne, or your acne is triggered by a hormonal surge (fluctuations or abnormalities), genetic predisposition, lifestyle factors such as diet, stress, medications as so on, what is basically taking place in your skin is as follows;
- inflammation
- excess oil (also called sebum) production in your pores
- clogged skin cells in your hair follicles
- and increase in acne-causing bacteria called Propionibacterium acne (more recently called Cutibacterium acne.
TEEN ACNE OR ADOLESCENT ACNE

For many people (male or female), acne begins when they hit puberty and it is called adolescent acne (also referred to as teen acne).
The onset of teen or adolescent acne may be confusing for so many but you are not alone as statistics show that over 85% of teenagers suffer teen acne.
Adolescence acne occurs because your body goes through many changes, one of which is an increase in your level of androgenic hormone (testosterone) – androgen is what stimulates your sebaceous gland to produce sebum.
An increase in androgen can cause excess production of oily substances (called sebum) that can clog your pores and lead to acne.
Note that after going through adolescence – usually between 10 and 19 years according to the UN – your acne breakouts may remit.
Presentation of Adolescence Acne
Adolescence acne can present as whiteheads, blackheads, papules, and pustules and usually appear on the face, neck, upper back, and chest.
PERSISTENT, RECURRING AND LATE ONSET OF ACNE
Persistent acne
For those adolescents whose acne breakouts fail to remit and continue into adulthood, your acne becomes persistent acne. And among a small percentage of sufferers, it could persist even after 50 years of age, says Bagatin et al..
Recurring acne
For those adolescents who enjoy a period of remission of their acne but later suffer a reappearance of acne breakouts in adulthood, your breakout is termed recurring acne.
Late Onset (in adulthood)
This class of acne sufferers never experienced acne during adolescence. However, they suddenly start to have breakouts during adulthood, starting after 25 years of age.
This is usually caused by high levels of androgen that your body produces during this period due to adrenal or ovarian factors such as PCOS and pre-menstruation (in females) or synthetic steroids (taken by mostly males). Genetic predisposition, cosmetics, stress, and smoking can also contribute to late onset of acne in adulthood.
ADULT ACNE
Hormonal Acne As a Type of Adult Acne/Adult Female Acne

Adult acne is more common among adult females than males, affecting about 76% of women compared to males, as reported by Bagatin. The onset of adult acne is said to be from 25 years of age. Among females, this is called adult female acne.
Factors that may contribute to adult acne in females include;
- Genetic predisposition
- PCOS (accounting for majority of cases),
- Menstruation.
- Stress
- Lifestyle such as smoking, diet, medications cosmetics.
For males, contributing factors may be;
- Genetic predisposition,
- Stress
- Lifestyles such as smoking, diet, medications, and synthetic steroid,
as identified by Skroza et al.,
Read more to find out how lifestyle factors, especially diet influence the onset of acne.
Adult Female Acne – Two categories include;
1) Premenstrual or Cyclical acne
Occurs in the days before menstruation and is due to hormonal fluctuations during your menstrual cycle, usually between ages 25 and 44. Premenstrual acne flare-up is more significant over 30 years of age, reported Zeichner et al..
This type of acne is what many people erroneously referred to as “hormonal acne”, as all acne is mediated by hormones. However, a more appropriate term for it would be premenstrual acne or cyclical acne, says Zeichner et al..
2) Perimenopausal acne (just before menopause)
This usually occurs from 45 years of age just before menopause. At this stage, there is a dip in your estrogen, creating a hormonal imbalance that can cause your androgen (testosterone) ratio to be higher relative to the falling level of estrogen. As a result, you will notice a flare-up of acne.
Presentation of adult female acne
Adult female acne (hormonal acne) occurs on the lower part of your face, your jaw line and around your mouth – referred to as the “hormonal belt”.
However, you can also find that some female populations with hormonal acne can have a distribution of lesions on their neck, upper back, and chest.
You will notice that you tend to have more inflammatory acne and fewer comedones (i.e. whitehead and blackhead) than adolescent acne.
Its severity is usually mild to moderate, as explained by Skroza et al..
MILD, MODERATE, AND SEVERE ACNE
Although there are structured systems for grading acne such as the Global Acne Grading System (GAGS), Feldman et al. provided a concise and simplified definition of each severity of acne as follows;
Mild acne
It appears as a few red papules and pustules mixed with comedones (whitehead and blackhead). Less than half of the face is involved.
Moderate acne
It appears as many papules and pustules mixed with prominent scarring. More than half of the face is involved.
Severe
Appears as red papules and pustules as well as several deep-seated nodules that are extremely inflamed. The entire face is involved. And when it is very severe, the entire face is very inflamed with nodules
6 INDICATIONS FOR HORMONAL TREATMENT
When do you seek hormonal therapy? Elsaie says that the indication for hormonal therapy is as follows;
- If conventional treatment fails
- When your acne flares up severely prior to menstruation.
- Acne caused by PCOS.
- Late acne onset (also known as acne tarda).
- When oral contraception is what is desired as a suitable treatment.
- Hhyperandrogenism that results due to adrenal or ovarian causes
CONVENTIONAL TREATMENT FOR MILD TO MODERATE HORMONAL ACNE
As suggested by Elsaie above, conventional treatment does not include hormonal therapy.
While a trip to your dermatologist is recommended for treating severe acne and in some cases, moderate acne, see below available conventional treatments;
Gabatin et al. state that topical treatments are the most widely used and effective treatments for mild to moderate acne. Topical treatments can also be used as maintenance therapy.
The two major questions you want to ask are;
- Is it tolerable?
- Is it effective?
Available Prescriptions to Manage Hormonal Acne
Conventional treatments available by prescription from your doctor or dermatologist, as identified by Bagatin et al. include;
Topical treatments: Retinoids, topical antibiotics, benzoyl peroxide, azelaic acid, and dapsone.
Although effective for mild to moderate acne, some associated side effects include dryness and skin discomfort as seen with retinoids, photosensitivity and bleaching of cloth as seen with benzoyl peroxide,
Cons of conventional topical treatment: As for azelaic acid, systemic side effects does not occur unlike the others already mentioned, so it is considered a safe option during pregnancy and breastfeeding. They may also cause irritation, damage to your skin barrier, and water loss from your outer skin layer.
As for dapsone, it is a preferred option for maintenance therapy as it is unlikely to cause bacterial resistance like antibiotics.
Systemic treatment: Antibiotics such as tetracycline can be prescribed to treat mild to moderate acne.
Cons of systemic antibiotics: However, there is risk of bacteria resistance. Also, it is contraindicated for use during pregnancy as it can inhibit skeletal growth of fetus and cause dental changes.
Cosmeceutical and Cosmetics in treating Mild to Moderate Acne
Bagatin et al. explained that cosmeceuticals and cosmetics clinical data support the effectiveness of cosmeceuticals and cosmetics for treating mild to moderate acne, although they are not superior to prescribed treatments.
Evidence exists that cosmeceuticals and cosmetics can improve mild to moderate acne in 4 to 8 weeks, as reported by Bagatin et al.. However, selecting the right product is a challenge in the market of endless options.
9 benefits of cosmeceuticals and cosmetics treatments include;
1) There is clinical evidence that retinoids retinol and adapalene 0.1%, as well as niacinamide, vitamin B3 and glycolic acid can be used to initially treat mild to moderate acne including whiteheads, blackheads, as well as seborrhea, reported Bagatin et al..
2) Niacinamide is also shown to be effective as an antimicrobial, sebostatic and anti-inflammatory agent. It can also help to increase the production of ceramides, prevent nitric oxides, and enhance kin barrier function.
3) Cosmeceuticals and cosmetics’ active ingredients can also help to reduce excess oil (sebum) production and reduce pigmentation such as glycolic acid.
4) Active ingredients in cosmeceuticals and cosmetics can also help to unclog pores and minimize the appearance of pores.
5) They can also help to provide radiant, smooth and soft skin
6) Cosmeceuticals and cosmetics have active ingredients included in cleansers, toners, serums, moisturizers, and sunscreens that can help to treat hormonal acne, used as mono therapy and as maintenance treatment.
7) You can easily incorporate this into your daily skincare routine, thereby improving adherence to treatment.
8) When you use makeup as camouflage, it can also be shown to improve adherence and the quality of life of acne sufferers.
9) Better tolerated
4 Cons of cosmeceuticals and cosmetics
1) Available without prescription and supervision.
2) Can worsen acne, as in the case of makeup, therefore it is important to select products that are labeled non-comedogenic.
3) Excessive use of cosmetics can worsen acne as well.
4) Selecting the right product is a challenge in a market of endless options.
OTHER FORMS OF THERAPIES FOR HORMONAL ACNE AND SCARS
You may need to consult with your doctor or dermatologist to discuss your desire for the following therapy options;
Some therapies for hormonal acne and scars include
- Eletrocauterization of macro-comedones.
- Draining of cysts and abscesses.
- Microdermabrasion.
- Chemical peels, lights, and lasers.
HORMONAL TREATMENTS
If all conventional treatments have failed and you meet the indications for hormonal therapy, as explained above, you may discuss this option including treatment plan, efficacy, and side effects with your doctor or dermatologist.
Some hormonal therapies
- Cyproterone acetate
- Flutamide
- Oral Contraceptive Pills (e.g. drospirenone)
SEVERE ACNE
Severe pustular and nodulocystic acne treated according to the European guidelines recommends hormonal treatment along with topical and systemic antibiotics as a preferred option to starting treatment with isotretinoin, says Elsaie.
DIET AND ACNE
When it comes to the influence of diet on acne formation, it is often a controversial one. Although there is some evidence that suggests that eating foods with a high glycemic index (GI) may increase your risk of breakouts while foods with low GI reduce your risk.
Read more about foods with high glycemic index
Also dairy that such as milk, yogurt and cheese may also increase your risk of breakouts. However, you do get a lot of benefits from these foods such as calcium for healthier and stronger bone. So cutting them out will be a great injustice to your system. A way to get around this may be to keep your dairy intake in moderation or considering alternatives fortified with calcium such as soy or almond milk may be worth considering.
Read more about the influence of diary on acne and alternatives
If you enjoyed or learned from reading this article, please leave a message on how you found this write-up. This is to encourage us and will help us know that you are there to read our content as we continue to provide high-quality materials for your pleasure!
REFERENCES
Bagatin, E., Freitas, T., Rivitti-Machado, M. C., Machado, M., Ribeiro, B. M., Nunes, S., & Rocha, M. (2019). Adult female acne: a guide to clinical practice. Anais brasileiros de dermatologia, 94(1), 62–75. https://doi.org/10.1590/abd1806-4841.20198203
Elsaie ML. Hormonal treatment of acne vulgaris: an update. Clin Cosmet Investig Dermatol. 2016;9:241-248. Published 2016 Sep 2. doi:10.2147/CCID.S114830
Feldman, S., Careccia, R. E., Barham, K. L., & Hancox, J. G. (2004). Diagnosis and treatment of acne. American Family Physician, 69(9), 2123-2130.
Skroza, N., Tolino, E., Mambrin, A., Zuber, S., Balduzzi, V., Marchesiello, A., Bernardini, N., Proietti, I., & Potenza, C. (2018). Adult Acne Versus Adolescent Acne: A Retrospective Study of 1,167 Patients. The Journal of clinical and aesthetic dermatology, 11(1), 21–25.
Zeichner JA, Baldwin HE, Cook-Bolden FE, Eichenfield LF, Fallon-Friedlander S, Rodriguez DA. Emerging Issues in Adult Female Acne. J Clin Aesthet Dermatol. 2017;10(1):37-46.